- 07736 104738
- sam@medicalmassagelady.com
- Mon - Sat, 8:00 - 18:30
I remember a few years ago, feeling around a bruised area on my shin & feeling lots of bumps along the length of my shin bone, & after doing some research, realising that my flat feet, frequent bruised feeling on my shins & tendency for tight calves all added up to one thing…shin splints(otherwise known as Medial Tibial Stress Syndrome or Medial Tibial Tenoperiostitis).
I see many clients who complain of shooting pain along the inner tibia (shinbone), usually in the middle/lower leg, while out running, to the point that they have to stop. This happens because the connective tissue (tenoperiosteum) that attaches the calf muscles to the tibia becomes inflamed, so when the calf muscles contract, they pull on the tenoperiosteum. If the tension is repetitive or forceful, this causes inflammation, pain & shin splints. Pain on the inner tibia is called medial shin splints, whereas pain felt on the outer tibia is called anterior shin splints.
RISK FACTORS:-
Those in the at risk group have a 4 - 35% chance of developing shin splints.
• women - several times more likely to suffer stress fractures from shin splints, due to increased diminished bone density & osteoporosis
• people who exercise regularly & hard
• athletes early in the season following a period of reduced activity
• athletes training on harder surfaces
• runners
• dancers
• military personnel
• people who have previously had shin splints
• overweight people
• people with tight calf muscles – can cause excessive pronation
• those who have had foot problems such as flat feet, high arches or plantar fasciitis
CAUSES:-
• OVERUSE & OVERLOADING OF THE LOWER LEG DUE TO BIOMECHANICAL ABNORMALITIES – increases stress on the tibia
- SUDDEN INCREASE IN INTENSITY/FREQUENCY OF ACTIVITY LEVEL – repetitive stress increases muscle fatigue & forces the tibia to absorb most of the impact, causing tibial bowing
- MUSCLE IMBALANCE - weak core muscles, weak hips or tightness of lower leg & plantar muscles, will affect the way that the shin bone absorbs the impact. Disruption of Sharpey's fibres, connecting the medial soleus fascia through the tibial periosteum will cause shin splint pain.
• EXCESSIVE ECCENTRIC MUSCLE ACTIVITY - the tibialis anterior muscle on the outer shin, is lifts the foot, lengthening to gently lower the forefoot after the heel strikes the ground ie. uses muscle contraction while lengthening.
• UNDERTAKING HIGH IMPACT EXERCISE ON HARD SURFACES - the impact of the foot landing on hard surfaces can increase muscle soreness following exercise, & contribute to the formation of chronic trigger points. Running uphill, downhill, or on uneven terrain, will increase the eccentric contraction, & therefore impact further.
• INAPPROPRIATE FOOTWEAR – wearing worn-out unsupportive shoes during exercise will increase injury risk & impact through the joints
• FLAT FEET- wearing supportive shoes & arch supports will help the impact to be distributed more evenly. Flat feet & plantar fasciitis can cause pulling of the shin tendons & consequently tears, which will result in inflammation.
• POOR EXERCISE TECHNIQUE – eg. overpronation of the feet when running increases the stress on the tibia, & can cause stress fractures, resulting in a bruised feeling & bumps along the shin
• ACTIVITIES KNOWN TO TRIGGER SHIN PAIN – dancing, running, military training
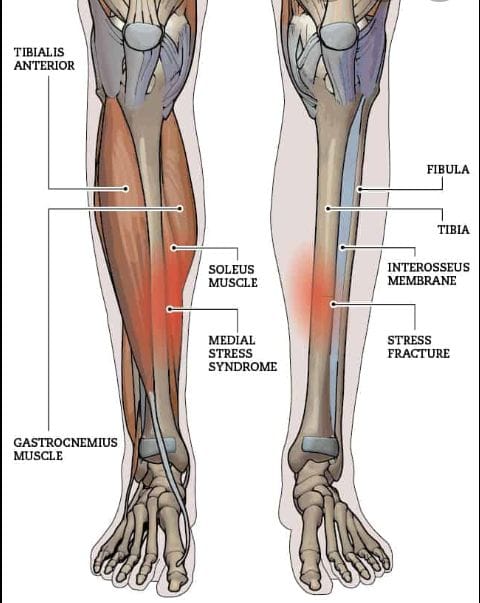
SYMPTOMS:-
- Muscle pain in one or both legs during or after exercise
- dull or sharp aching pain in the front lower leg, along inner border of the shin
- pain with activity that exerts pressure on the shin bone
- pain improves with rest
- occasionally localized swelling of the bone
- numbness & weakness in the feet
- stress fractures - in severe cases, walking with a limp, some inflammation of overlying skin, muscle tightness/thickening or lumps on the bone
DIFFERENTIAL DIAGNOSIS:-
Gentle pressure on the tibia will recreate the pain in shin splints, usually affecting over 5 cm length of the bone. While some localised swelling can occasionally occur, obvious signs of inflammation, poor pulse or rapidly developing severe pain on top of the usual shin splints symptoms will indicate a different underlying cause eg.:-
- stress fractures
- anterior compartment syndrome
- nerve entrapment
- popliteal artery entrapment syndrome
OTHER CONDITIONS WHICH MAY BE LINKED TO SHIN SPLINTS
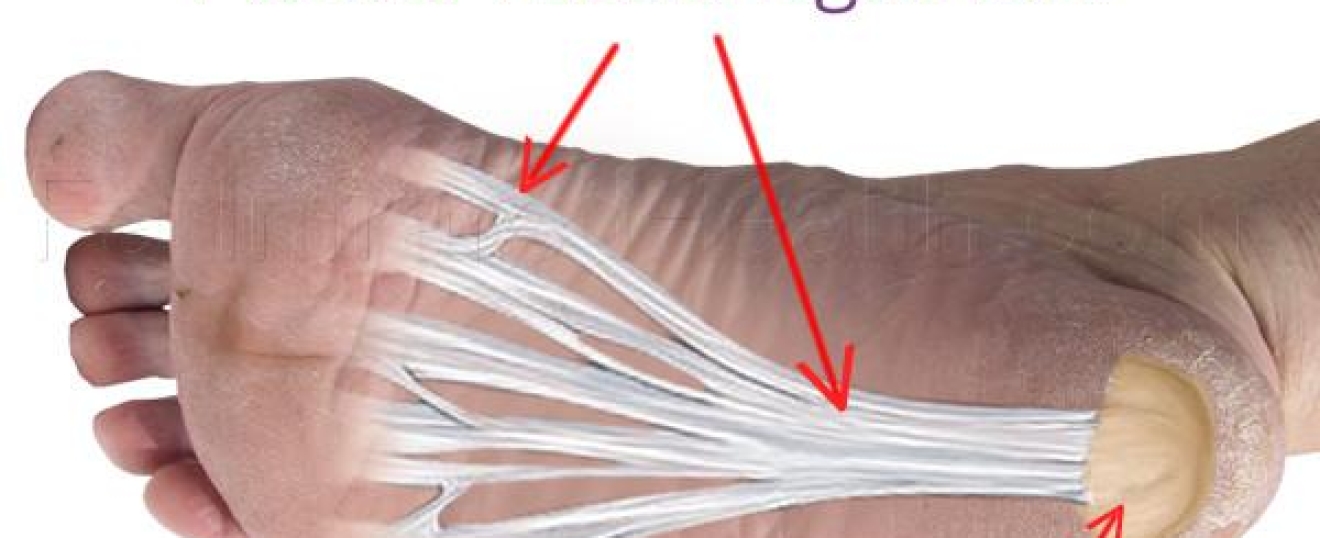
- PLANTAR FASCIITIS – I’m always explaining to my plantar fasciitis clients the importance of massaging the calf muscles, because the insertion point of the tibialis anterior muscle can be felt around the arch of the foot. This tendon helps to support the arch of the foot, so if the tibialis anterior muscle is fatigued or tight, not only will arch support suffer but it can pull on the plantar fascia.
- MORTON’S NEUROMA - a sensitive growth on a nerve between the bones of the foot which gets pinched, causing pain. Morton's neuromas occur in the referral zones for tibialis anterior trigger points.
TREATMENT:-
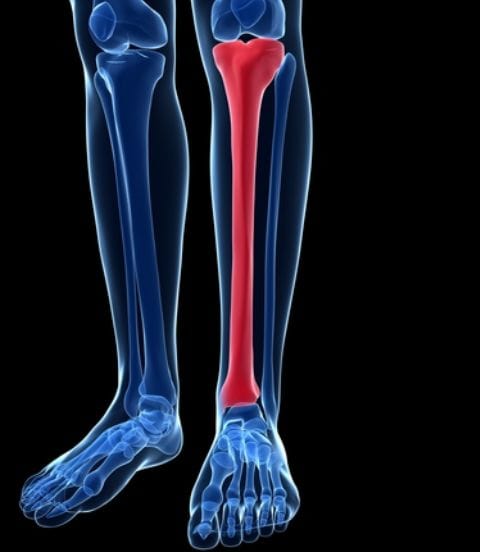
Recovery will be dependant on the severity & duration, & treatment available, but generally recovery periods of a few weeks to months will allow healing.
- rest followed by a gradual return to exercise – build up to previous level over a course of weeks to allow the tibia to recover from sudden, high levels of stress, decreasing activity if pain returns
- nonsteroidal anti-inflammatory drugs (NSAIDs)
- cortisone injections
- vitamin D & calcium supplements
- cold packs - to reduce inflammation & pain levels , 10 minutes 3-4 times a day
- physiotherapy - strengthening exercises once pain has subsided, on calves, quads & glutes, using a balance board
- massage therapy & joint mobilisation
- compression may be used
- shock absorbing insoles & arch supports to offset biomechanical abnormalities
- gradual return to exercise, starting with short, low intensity workouts. Cross training is recommended to maintain aerobic fitness
- cycling & swimming are good low impact exercises
- extracorporeal shockwave therapy (ESWT) for more severe shin splints
- surgery is rare – is last resort when other treatment for 1 year+ is ineffective
PREVENTION:-
- warm up thoroughly before exercising & stretch to cool down
- regularly stretch while exercising
- run on smooth, flat soft surfaces where possible, eg. grass, to reduce the impact on the tibia & calf muscles
- arch supports & shock absorbing insoles will help combat pronation & support the arch of the foot
- wear supportive footwear & replace running shoes regularly
- massage therapy
- reduce the intensity of training if symptoms start to develop
- massage roller stick for self-massage of the legs
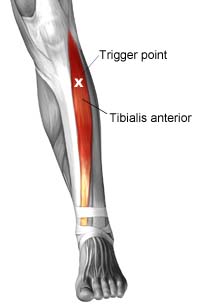
MASSAGE FOR SHIN SPLINTS
• can relax calf muscles & connective tissue – both front and back of the lower leg should be massaged as only treating the tibialis anterior will not help with tibial stress fractures
• can relieve pain
• can ease inflammation
• anterior compartment syndrome, caused by swelling of the compartment that the tibialis anterior muscles sits in, can destroy the muscle tissue & lead to potentially life-threatening infection. This can be helped by massage but if you have severe, rapidly developing shin pain, seek urgent medical attention.
TYPES OF MASSAGE
• SWEDISH MASSAGE – light to medium pressure on the muscles, will help to improve the circulation & lymphatic drainage of the metabolic waste away from the muscles
• DEEP TISSUE MASSAGE – stretches the muscles to ease tightness & relieve tension on the shin bone, relieving pain & reducing the formation of scar tissue
• SPORTS MASSAGE – accelerates healing by reducing post exercise recovery time. It works on the muscle-tendon junctions & helps improve flexibility to avoid the risk of injury. It will address muscle imbalances & biochemical abnormalities which place additional stress on the shin bone.
• TRIGGER POINT THERAPY – point pressure may calm the tibialis anterior muscle down enough to relieve chronic pain, without irritating the whole muscle & increasing the pressure in the muscle compartment. Latent trigger points in the upper third of the tibialis anterior muscle of the shin may increase in sensitivity. You can palpate your own tibialis anterior muscle by feeling the outer edge of the shin, where there is a thick pad of muscle starting about 5cm below the knee. The trigger points in the top third of the muscle are usually very potent & may radiates down the shin to the top of the foot.
• SELF MASSAGE - using massage oil slide your forearm or the heel of your hand up the length of the tibialis anterior muscle & this may hit the trigger points at the top of the stroke.
EXERCISES
You will want to focus on strengthening the calf muscles which surround the tibia, and you can find various calf stretches in my previous set of posts on the calf muscles. You can also try to reduce pain by doing some of the following basic foot exercises:-
1)with foot flat on the floor, alternate between lifting the toes off the floor and the heel. You can then progress this by lifting the heel off the floor and then lifting the toes at the same time.(dorsiflexion & plantar flexion)
2)lift toes off the floor and turn the foot outwards(dorsiflexion + eversion)