- 07736 104738
- sam@medicalmassagelady.com
- Mon - Sat, 8:00 - 18:30
Gluteal tendinopathy is the most common hip tendonitis and a common cause of Greater Trochanteric Pain Syndrome. Gluteal tendinopathy is often associated with trochanteric bursitis.
The gluteal tendons connect gluteal muscle to the hip bones, and injury is usually the result of numerous micro tears over time, often due to overuse.
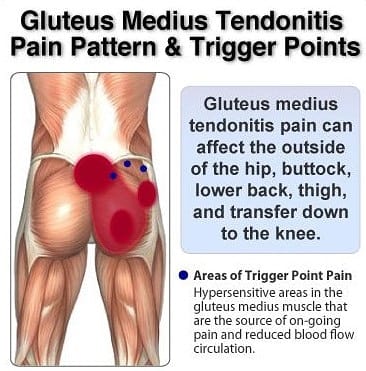
Tendon injuries occur in three areas:-
· musculotendinous junction (where the tendon joins the muscle)
· mid-tendon (non-insertional tendinopathy)
· tendon insertion (eg into bone)
Tendinitis means "inflammation of the tendon," but inflammation is a rare cause of tendon pain. The most common form of tendinopathy is tendinosis, a noninflammatory degenerative condition that is characterised by collagen degeneration in the tendon due to repetitive overloading. Therefore tendinopathies do not respond to anti-inflammatories but rather functional rehabilitation.
CAUSES:-
· gradual wear and tear to the tendon from overuse or ageing
· repetitive movements through occupation, sports, or daily activities
· stress on the tendon due to heavy loads causes small micro tears, which encourage inflammatory chemicals and swelling. If the stress continues damage will exceed the rate of repair causing pain and dysfunction · poor hip and gluteal muscle control that leads to overstressing of the gluteal tendons, causing pain and hip-pelvis instability
· continued hip instability which may lead to trochanteric bursitis
SYMPTOMS:-
·- lateral hip pain
- may increase overnight or early morning
·- stiffness
- may increase overnight or early morning
·- loss of strength
·- tender, red, warm, or swollen if there is inflammation
·- crunchy sound or feeling when you use the tendon ·
- pain may worsen when you using the tendon eg running
·- pain is often worse when you lie on the affected hip
The symptoms of a tendinopathies are similar to bursitis.
STAGES OF TENDINOPATHY:-
If a tendon can’t adapt to the load placed upon it, it will progress through four phases of tendon injury. Progression past stage 1 can cause cell death and tendon rupture.
1. REACTIVE TENDINOPATHY
· normal tissue adaptation phase
Prognosis: Excellent
2. TENDON DISREPAIR
· Injury rate exceeds repair rate
Prognosis: Good. Tissue is attempting to heal.
3. DEGENERATIVE TENDINOPATHY
· cell death occurs
Poor Prognosis - Tendon cells are wearing out
4. TENDON RUPTURE
· catastrophic tissue breakdown
· loss of function
· surgery is often the only option
Prognosis: very poor Identifying the correct phase is essential to finding effective treatment, as different options should be undertaken in specific tendon healing phases.
TREATMENT:-
· rest the painful area, and avoid activities that increase pain
· apply ice or cold packs for 20 minutes at a time, as often as 2 times an hour, for the first 72 hours
· gentle range-of-motion exercises and stretching to prevent stiffness
· physiotherapy
· massage
· eccentric strengthening program
· ultrasound
· steroid injection if recovery is slow
· hip surgery in severe cases
As previously stated, anti-inflammatories may not be effective in tendinopathy.
RETURN TO SPORT:-
· requires clearance by physiotherapist
· build back to your previous level slowly, and stop if painful
· warm up before you exercise
· apply ice after activity to prevent pain and swelling
· continue your hip stabilisation exercises
· full rehabilitation may take weeks or months