- 07736 104738
- sam@medicalmassagelady.com
- Mon - Sat, 8:00 - 18:30
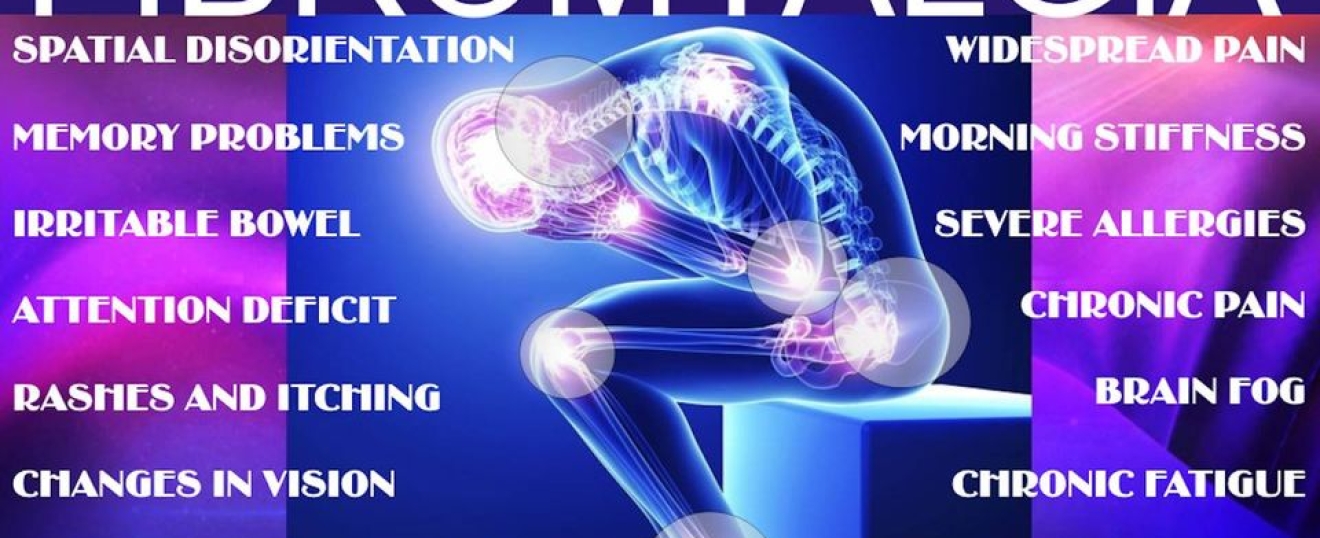
WHAT IS FIBROMYALGIA?
Fibromyalgia is a condition that causes pain throughout your body. It also leads to fatigue, sleep issues, and other symptoms. People with this condition are more sensitive to pain than those without the condition.
Fibromyalgia is one of the most common chronic pain conditions in the world. It affects over 20,000 people per year in the UK, according to the National Fibromyalgia Association (NFA).
The cause of fibromyalgia is still a bit of a mystery. But there is research that points to several factors that may be involved. The research also includes risk factors that may increase a person’s chance of developing the condition.
Clients with fibromyalgia often have a dual diagnosis of osteoarthritis, hypothyroidism or lupus.
They are also more likely to have other major medical issues such as heart attack, high blood pressure, diabetes, depression & other mental illness & rheumatoid arthritis.
CAUSES
Suggested causes include:-
• ABNORMAL PAIN SIGNALLING - the nervous system may not process pain signals in the usual way, increasing pain sensitivity, due to abnormal levels of chemicals in the brain, spinal cord, and nerves
• HORMONE IMBALANCES – relatively low levels of hormones such as serotonin, norepinephrine (noradrenaline), in the brain and nervous system, which help the body to process pain, may interrupt pain signals and intensify your sensitivity to them
• GENETICS - fibromyalgia can run in families, probably due to an unidentified genetic abnormality increasing the risk for the condition. Certain genes may control the way the body regulates pain responses. Scientists speculate that people with fibromyalgia carry one or more genes that cause them to react strongly to stimuli that another person may not perceive as painful
• TRIGGERS - unlikely to cause fibromyalgia by themselves, but may trigger the onset in people who are already at risk for it by altering the nervous system’s response to pain, eg. - infections such as the flu - repeated injuries - surgery - emotional trauma eg.break up, divorce, or the death of a loved one - childbirth
SLEEP DISTURBANCES - Problems getting enough sleep or spending enough time in the deepest stages of sleep are common in this disorder. But doctors aren’t sure if this is a symptom or a cause of fibromyalgia. Abnormal sleep patterns can affect the levels of some brain chemicals.
RISK FACTORS
• GENDER - more common in women than in men, women are eight to nine times more likely than men to have fibromyalgia. Scientists believe that women experience pain differently, partly due to reproductive hormones, such as oestrogen, which make women more sensitive to pain, hence why pain levels fluctuate during a woman’s menstrual cycles when oestrogen levels rise and fall. Menopause, which also results in lowered levels of oestrogen, is another potential risk factor for fibromyalgia. • AGE - most people are diagnosed in early to middle adulthood, between the ages of 20 and 50
• FAMILY HISTORY - having a close family member with fibromyalgia, increases the chance of being diagnosed yourself
• SLEEP DISORDERS - It’s not known if sleep problems are a symptom or a cause of fibromyalgia. Some people who have disorders affecting sleep, such as sleep apnoea and restless leg syndrome (RLS), are more likely to have the condition
• OTHER RHEUMATIC DISEASES - Rheumatic diseases affect the joints, muscles, and bones. People who have another rheumatic disease are more likely to have fibromyalgia eg. - rheumatoid arthritis (RA) - osteoarthritis (OA) - lupus - ankylosing spondylitis
• DEPRESSION - Mood disorders and fibromyalgia are closely related. Mental health conditions such as depression and anxiety stem from the same chemical imbalances linked to fibromyalgia. The strain of living with chronic pain can also cause depression. Also, depression can make your pain worse
• EXERCISE – too much or too little
• SURGERY
SYMPTOMS:-
• dull, aching pain on both sides of your body and above and below your waist
• tenderpoint pain around the soft tissues of the joints
• fatigue
• flu like symptoms
• trouble remembering and concentrating, sometimes called “fibro fog”
• trouble sleeping
• headaches
• tight upper neck
• jaw pain or clicking
• depression and anxiety
• diarrhoea and abdominal pain
• painful menstrual periods
• numbness or tingling in the hands and feet
• sensitivity to noise, light, or temperatures (hot or cold)
HOW DOES MASSAGE HELP?
Starting with softer more relaxing strokes to warm up the muscle tissue, followed by deeper frictions over knots to relax the muscles & break down the thickened fibres of connective tissue, release toxins & reduce pain, the following benefits can be seen:-
- Increased serotonin levels (mood enhancing hormone)
- Decreased circulating cortisol & adrenaline levels (stress hormones)
- Decreased levels of substance P (a pain messenger)
- Decreased tenderpoint pain
- Improved sleep patterns
-Improved overall wellbeing & elevation of mood
FIBROMYALGIA TENDER POINTS
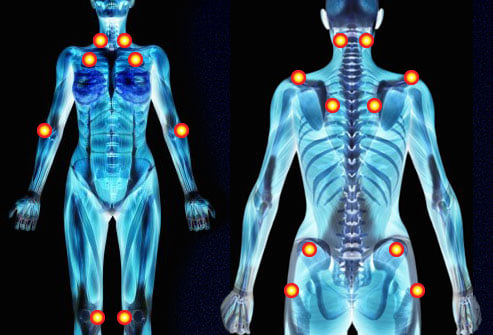
Tender points, of which there are 18, can be confused with trigger points, and will produce localized pain when pressed. It has been suggested that these tender points, which are around the size of a penny, are due to hyperstimulation of the central nervous system. Tender points are located in clusters around the neck, chest, shoulders, elbows, hips, and knees, and are located on both sides of the body.
In the past, diagnosis of fibromyalgia has been dependant on having at least 11 out of the 18 tender points for 3 months or more, covering all four quadrants of the body. One cause of fibromyalgia previously being undiagnosed, is that people with fibromyalgia have fluctuating pain levels, so may have only had pain in a few points on the day of their doctors appointment.
Now other factors such as cognitive symptoms, fatigue, sleeping patterns and a pain index are used in diagnosis. This gives a more accurate indication of fibromyalgia, since tender points are very close to trigger points which can also be an issue for sufferers. Trigger points are hard, knotty lumps that form in muscles causing localised and referred pain, whereas tender points, only cause localized pain. Trigger points and myofascial pain are very common in people with fibromyalgia, particularly in the neck and shoulders, where they tend to be more responsible for pain than tender points. Trigger points in fibromyalgia sufferers should be treated with limited intensity and duration, so as not to worsen the symptoms.
Overcoming pain and sensitivity in fibromyalgia tender points involves a number of methods:-
• Gradually building up from very light pressure on trigger points to a light massage or manual lymphatic drainage
• acupuncture
• Self treatment eg using bath brush in the shower over trigger points to desensitize
• Stretching
• Correcting underlying factors
Ensure that you see a therapist who is qualified and experienced in dealing with fibromyalgia.