- 07736 104738
- sam@medicalmassagelady.com
- Mon - Sat, 8:00 - 18:30
“It is more important to know what sort of person has a disease than to know what sort of disease a person has.” (Hippocrates)
This statement is still relevant today when treating some clients. It is a common belief that pain is caused by some kind of physiological dysfunction, but for up to around 40% of people, pain is psychosomatic, which doesn’t mean that the person is imagining it, just that there may not be an obvious biological cause. These are the cases where medications don’t work, tests come back clear and numerous referrals to various professionals may be made.
Progression of disease and tissue damage may not be the cause of pain
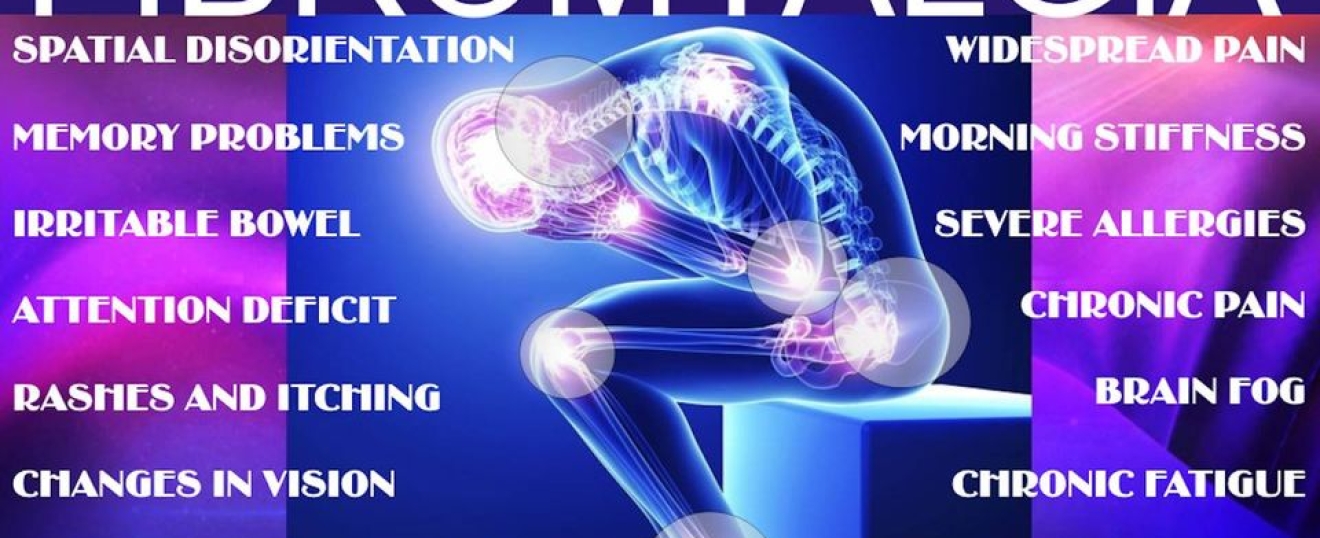
The correlation between pain and disease progression or the extent of an injury, based on the view that the nerves transmit pain signals to the brain, can be a common misconception. Examples of where this correlation is shown to be untrue can be seen in clients with IBS, fibromyalgia or amputees with phantom limb pain. In these cases, there is no sign of tissue damage, or even pain receptors.
If I think about some of my gym clients, pain can be a protective mechanism against injury, warning them not to push themselves any harder. Our sensory nerves feed the brain with information about tissue damage, inflammation, temperature etc, via nociceptors (sensory neurons), which detect danger and which may be tied into our memories. This means that we can anticipate pain before it happens, for example, in clients with PTSD, where triggers stimulate the sympathetic nervous system.Therefore….
Chronic Pain can be a sign of constant danger
But that can’t be true can it? Every person who suffers from fibromyalgia, for example, isn’t constantly at risk of injury. However, we often repress emotions that we feel unable to deal with, as is commonly the case with trauma and PTSD, but can also be true of any strong emotions such as grief or anxiety, and the unconscious brain is unable to differentiate between physical and psychological danger.So….
Chronic pain feeds off fear
is why so many people with PTSD also suffer with chronic pain. Emotions from the initial trauma have been buried but the nociceptors still sense danger. Fear of an initial pain can trigger something in the unconscious part of the brain, often causing us to have fear that we may not be able to explain. This fear can then show itself as physical pain, where there is no biological sign of disease or injury. When people then start to worry about when the pain will end, this exacerbates the fear and a pain cycle begins. The sympathetic nervous system then takes over, releasing adrenaline and cortisol, which induce the fight or flight response. When the body is in this state for a long period, it brings about central sensitisation of the nervous system, meaning that the neural pathways work overtime, overstimulating the brain, which will incorrectly interpret normal sensory signals as a perceived threat
.By undertaking regular exercise, deep breathing and having regular massage treatments, it is possible to replace sympathetic nervous system dominance with the parasympathetic, which will calm everything down and rebalance the nervous system, thus helping to reduce overloading of the brain with sensory signals.