Fascia Dysfunction and Myofascial Pain Syndrome

Myofascial pain syndrome affects over 20,000 people each year in the UK. It is a chronic muscular pain disorder, affecting the fascia (connective tissue surrounding the muscles), where trigger points cause pain throughout the muscle, and also referred pain to other areas, sometimes for periods of several months. It usually develops following repetitive contraction of a muscle, due to work, hobbies or stress.
THE ROLE OF FASCIA IN PAIN AND DYSFUNCTION
• fascia surrounds nerve endings as well as muscles, so can displace joints and irritate nerves
• fascia impacts on circulation, potentially reducing blood flow needed for the soft tissues to be healthy, since arteries and veins run through the soft tissues and therefore, the fascia
• fascia controls synthesis of collagen and hyaluronic acid, which are needed for cellular repair
• fascia has its own pain receptors and can thicken in response to chemical messengers eg. fear, cortisol
Therefore, fascia plays an important role in soft tissue pain and healing, and in trauma/stress induced physical pain.
DYSFUNCTIONAL FASCIA:MOST COMMONLY INJURED FASCIA:-
• plantar fascia - covers most of the arch of the foot
• IT band - on the outer thigh
• lumbodorsal fascia - on each side of the lower back, connecting the bottom of the rib cage to the pelvis
Tension and spasms in the fascia, and reduced fascia length, result from broken or additional crosslinks in the injured collagen, that tend to arise during the healing process. This tightness restricts the blood flow and waste products accumulate ie. inflammation.
Fascia dysfunction doesn’t occur in isolation and surrounding muscles/tendons/ligaments often suffer micro tears.
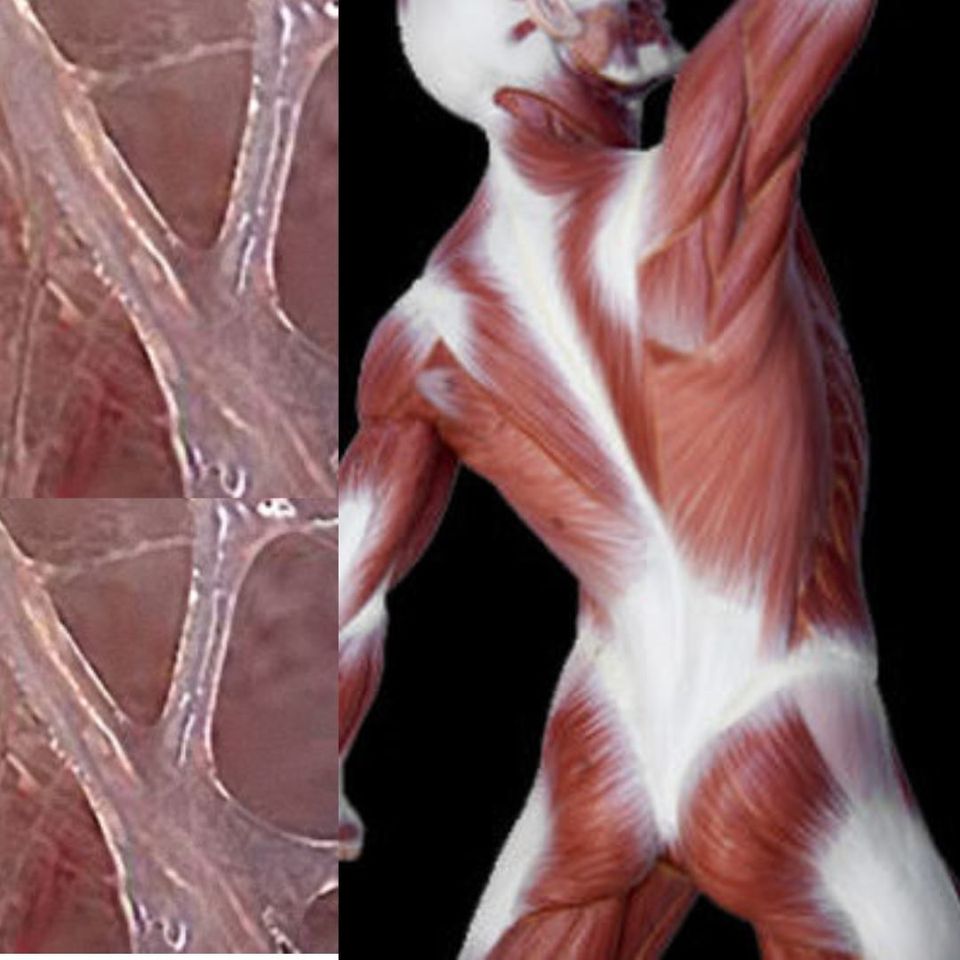
RISK FACTORS:-
The risk of developing myofascial pain syndrome is increased by anything that sets off trigger points
• MUSCLE INJURY - acute injury or repetitive muscle stress may encourage trigger points eg. a strained muscle or poor posture
• STRESS – regular/long term stress is more likely to result in sustained muscle clenching, which leaves muscles susceptible to trigger points
CAUSES:-
• poor posture
• emotional disturbances
• injury to muscle fibres
• repetitive motions
• lack of activity eg. sedentary lifestyle, a broken arm in a sling
SYMPTOMS:-
• deep, aching pain in a muscle/back/mouth
• pain that persists/worsens
• tender knot in a muscle
• muscle spasms
• disturbed sleep due to pain
• depression
• fatigue
• behavioural disturbances
If the muscle pain doesn't subside despite the usual self care measures and rest then it is time to see either a sports therapist or doctor, who will apply pressure to the painful area to feel for tension or muscle twitches, in order to identify any trigger points.
• active trigger point - an area of extreme tenderness within the muscle, associated with local pain
• latent trigger point – an inactive area that has the potential to become active, and may cause muscle weakness or restricted movement
COMPLICATIONS:-
Research has suggested that myofascial pain syndrome may potentially play a role in the brain becoming more sensitive to pain signals over time, which can develop into fibromyalgia.
TREATMENT:-
There is no solid evidence supporting any given therapy, and you will probably need to try a combined approach to relieve pain, but exercise is important in any treatment program.
• MEDICATION:-
- analgesics – to relieve pain
- nerve pain medication - blocks pain due to damaged nerves
- muscle relaxants - reduce muscle tension and help relieve muscle pain
- antidepressants - help reduce pain and improve sleep. Some antidepressants also help relieve pain
- sedatives - relax muscles and help reduce the anxiety and poor sleep that accompany myofascial pain syndrome
• INJECTIONS – cortisone injections into a trigger point
• ACUPUNCTURE
• DRY NEEDLING - inserting a needle in and around the trigger point may help break up the muscle tension
• ICE AND ELEVATION– ice packs for 15 minutes per hour, with elevation during inflammatory phase. Compression may help control swelling between ice sessions
HEAT - hot packs can help relieve muscle tension and pain
• ULTRASOUND - sound waves increase blood circulation and warmth, which may promote healing in muscles
• MOBILITY AIDS - use crutches if walking increases pain
• STRETCHING - a physiotherapist/sports therapist can guide you through gentle stretching exercises to ease pain in the affected muscle and joint, most likely starting with isometric strengthening. Strengthening the muscles surrounding a trigger point will help avoid overworking any particular muscle.
• FOAM ROLLER/THERACANE – if still experiencing spasms after several days
• PHYSIOTHERAPY - can devise a plan to help relieve your pain based on your signs and symptoms
• POSTURE TRAINING - improving your posture can help relieve myofascial pain, particularly in your neck
• MASSAGE (TRIGGER POINT THERAPY, MYOFASCIAL RELEASE & ROCKBLADING) - may help relieve pain and release tension and increase circulation to promote healing, plus release scar tissue that may be activating a trigger point, regulate the nervous system, reduce stress and depression and promote sleep. Soft tissue mobilization or myofascial release will promote post injury tissue remodelling and help restore normal tissue length.
PREVENTION:-
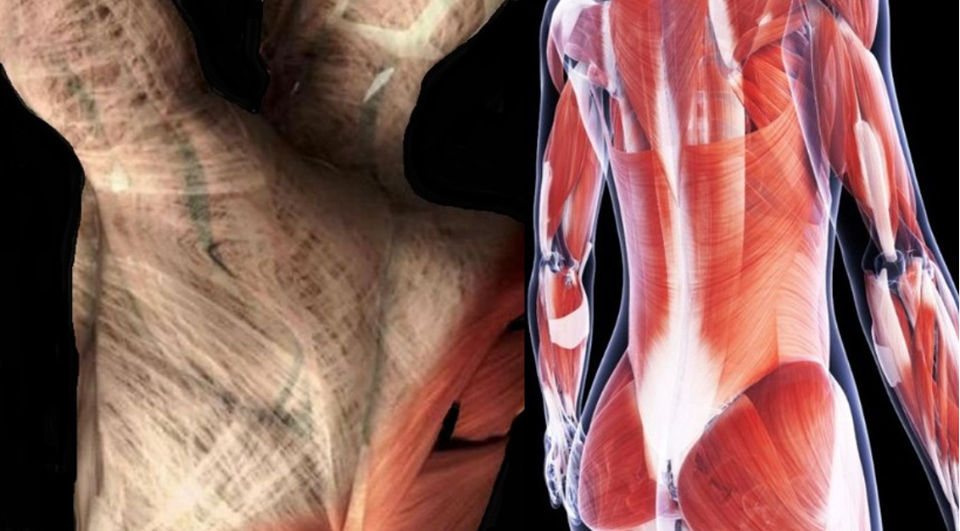
• prepare the tissue adequately through functional warm-ups prior to exercise
• maintain fascia length throughout the year
• appropriate intensity during training – any weekly increase in distance/speed/weight should not exceed 10% (and only increase 1 variable each week)
• stretching after exercise
• use ice packs if sore after exercise
Recent research shows that actin in the fascia brings about small contractions that send impulses to the fibroblasts, which regulate collagen production. This conditions the fascia, maintaining its density, resistance and mobility. Pain receptors are also present in the fascia, which could suggest that disturbances in the regulation of collagen production could be the cause of myofascial dysfunction. This would not only alter the circulation within the fascia and mechanical tension, but would also stimulate the pain receptors, which if they perceive as a harmful stimulus, will initiate the stress responses in the body. Changes in temperature and mechanical stress introduced by massage techniques will also affect the viscoelastic substance in which collagen is dispersed. As therapists, therefore, we must address fascia dysfunction and evaluate our treatment techniques accordingly, in order to maintain homeostasis.
