- 07736 104738
- sam@medicalmassagelady.com
- Mon - Sat, 8:00 - 18:30
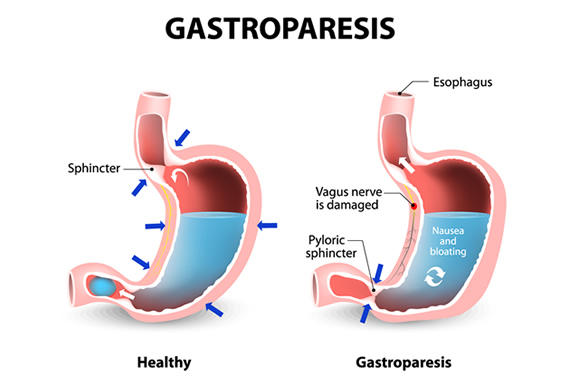
Gastroparesis, or delayed gastric emptying, means that food remains in the stomach for longer periods of time because it is unable to pass easily into the small intestine. This happens when regular stomach contractions to push partially digested food into the intestine dysfunction due to a damaged vagus nerve, and so further digestion and absorption of nutrients can’t happen. Dysfunctional muscles of the stomach and intestines can prevent movement completely.
Gastroparesis occurs in 10 men and 40 women per 100,000. Research has shown cumulative gastroparesis in 5.2% of Type1 and 1% of Type 2 diabetics, as opposed to 0.2% of non-diabetic people. Diabetes can cause gastroparesis due to its effects on the nervous system, with the vagus nerve, which controls the movement of food through the stomach. being commonly damaged. Blood sugars and quality of life in the diabetic will be influenced by delayed gastric emptying, gastric dysrhythmia, pylorus spasm and non-synchronized gastroduodenal motility.
RISK FACTORS
- type 1 diabetes
- type 2 diabetes for over10 years
- having coexisting autoimmune diseases
- history of certain gastric surgeries involving oesophagus, stomach, or small intestine which may affect the vagus nerve
- more common in females than males
- certain cancer treatments, eg. radiation around the chest or stomach area
CAUSES
- diabetes mellitus - high blood sugar affects the health of nerves throughout the body and can damage the vagus nerve
- impairment/surgical damage to the vagus nerve
- infection
- seizures
- tumours,
- chemotherapy and radiotherapy around chest/stomach
- hyperglycaemia delays stomach emptying
- diseases that cause damage to the stomach muscles eg.scleroderma, Parkinson’s disease, multiple sclerosis
- dysfunctional reflexes of the nervous system
- certain medications eg. narcotics, anticholinergics which block nerve signals, tricyclic antidepressants, calcium channel blockers, clonidine, dopamine agonists, lithium, nicotine, and progesterone
- hypothyroidism
- metabolic disorders
- mineral imbalances
- there may be no obvious cause ie.idiopathic gastroparesis – young and middle aged women are most at risk
- pyloric dysfunction
- certain psychological disorders
- eating disorders
- gastroesophageal reflux disease (GERD).
GENERAL COMPLICATIONS
- bacterial infections
- indigestible masses which cause stomach obstruction
- electrolyte imbalance
- oesophageal tears from chronic vomiting
- oesophageal inflammation which may cause difficulty swallowing
- severe dehydration, due to vomiting
- malnutrition due to poor absorption
- blood sugar abnormalities
- hardened, undigested food that can form a solid mass, which can become life-threatening
- bacterial overgrowth in the stomach due to undigested food
- reduced quality of life
COMPLICATIONS SPECIFIC TO DIABETICS
Gastroparesis can be very unpredictable which can cause difficulty in knowing when to take insulin and consequently blood sugar levels may rise or drop.
High blood sugar levels will increase the risk of:-
- kidney damage
- eye damage, such as retinopathy and cataracts
- heart disease
- foot complications that can lead to amputation
- neuropathy
- ketoacidosis
Whereas low blood sugar levels may cause:-
- shakiness
- diabetic coma from low blood sugar
- loss of consciousness
- seizures
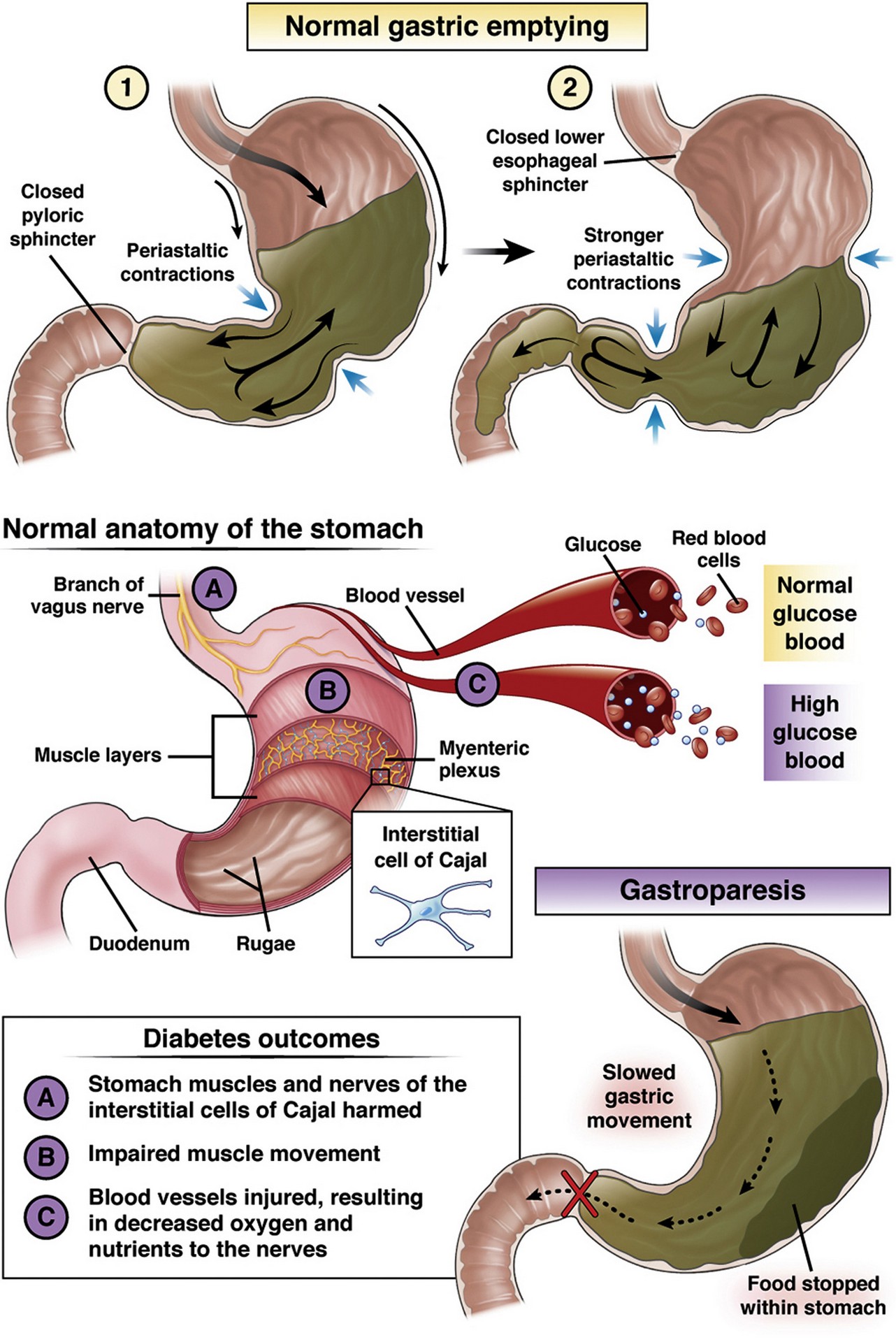
Symptoms can be mild or severe, but often worsen with solid fatty foods, and high fibre foods and fizzy drinks
- .nausea
- vomiting – often 2 hours after eating with undigested food particles
- lack of appetite
- feeling full much quicker
- pressure under the ribcage
- abdominal bloating
- upper abdominal pain and spasms which may be debilitating
- unintentional weight loss due to malnutrition (poor absorption of nutrients or low calorie intake)
- heartburn and acid reflux (GERD) - food starts to ferment when it sits in the stomach longer than it should, placing pressure on the lower oesophageal sphincter, potentially leading to sphincter dysfunction and acid reflux
- unstable blood sugar levels
Some conventional medical treatments can cause side effects and cardiac arrhythmia, local infection, malnutrition, and weight loss are inevitable, but the use of massage in combination with these treatments can help to reduce side effects and some symptoms.
TREATMENT
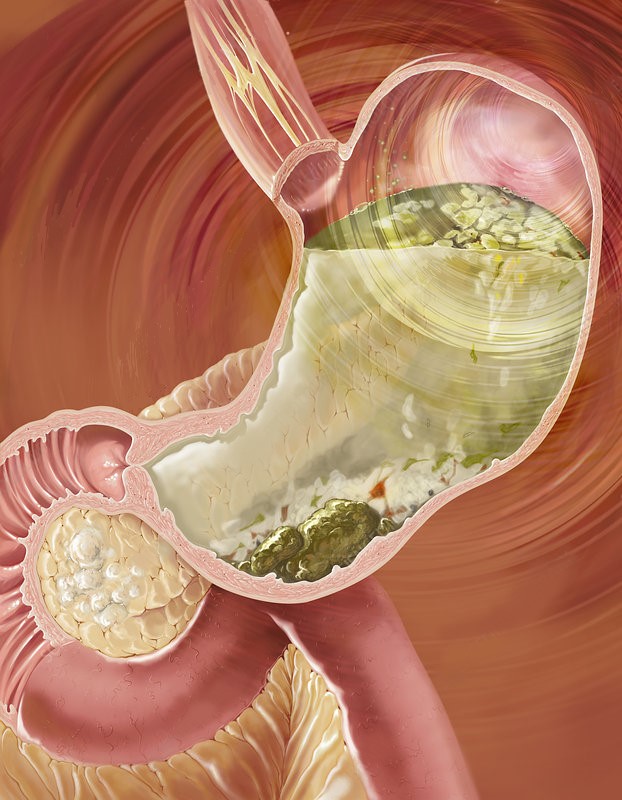
Treatment involves dealing with the underlying cause of gastroparesis rather than simply addressing the symptoms
MEDICATION :-
- metoclopramide to help stimulate the stomach muscles to contract helping the stomach to empty
- medications to reduce nausea eg. prochlorperazine, diphenhydramine or ondansetron
- avoid drugs that may delay gastric emptying eg. opiates
- antibiotics eg.erythromycin may be recommended if there is infection
- injections with Botulinum toxin (Botox) to help rest the bowel and increase emptying
DIET AND NUTRITION
- changes in diet and eating habits in severe cases
- where blood sugars remain uncontrolled, a temporary feeding tube or intravenous nutrition may be recommended to bypass the stomach and directly send nutrition into the intestine, keeping blood sugar levels stable
BLOOD GLUCOSE MONITORING
checking blood sugar levels more often will make it easier to decide on treatment, and may also involve altering the dosage and timing of insulin
ELECTRICAL GASTRIC STIMULATION
electrodes are attached to the stomach to trigger contractions
NATURAL REMEDIES
- ginger accelerates gastric emptying (recommended dose 3 x 1200mg) and may help with nausea
- visceral manipulation-massage to release stress and tension from abdominal organs and help to promote peristalsis
- acupuncture and acupressure may also help
MASSAGE
Abdominal massage has been shown by research to improve anorexia, bloating and epigastric pain in diabetic gastroparesis.
Acupressure (on ST36 and RN12) has also contributed to decreasing blood glucose and facilitating gastric emptying.
While research hasn’t shown any significant improvement with belching, nausea or vomiting, it is possible that adding aromatherapy to a colonic massage may help with this.
DIETARY SELF HELP
Recommended dietary adjustments include:-
- eating frequent, smaller meals instead of three larger meals each day
- reducing high-fibre foods which take longer to digest
- reducing fatty foods
- eating well-cooked vegetables instead of raw vegetables
- avoiding alcohol and carbonated drinks
- avoiding raw or uncooked fruits and vegetables
- avoiding fibrous fruits and vegetables
- eating liquid foods such as soups or pureed foods
- drinking water during meals
- gentle exercise following meals, such as walking
- avoiding fizzy drinks, smoking, and alcohol
- not lying down within 2 hours after eating
- warm meals are generally digested better than cold
- eat your meals in a relaxed environment as anxiety can slow digestion by up to 36 hours
- avoid cold beverages with meals
- chew your food well so that the digestive enzymes can reach the fine particles to break them down
- smelling your food to stimulate the digestive juices will prepare the stomach for the incoming food
OTHER SELF HELP MEASURES
- address any underlying causes eg. medication, hypothyroidism, diabetes
- talk to a functional nutritionist about diet to reduce the load on your stomach while ensuring adequate nutrition
- go for a relaxing walk after meals and avoid laying down to assist with emptying the stomach through gravity and stimulate the stomach and spleen meridians which run through the legs
- do vagal nerve stimulating exercises
OUTLOOK
People with diabetic gastroparesis are likely to have:-
- more hospital visits
- additional diabetic complications eg. eye damage, kidney damage and heart disease
The outlook will vary between individuals but effective blood sugar control gives the best chance of a positive outlook.