Massage for the client with a Stoma

There are approximately 120,000 people in the UK with some kind of stoma. Often stomas are temporary, allowing time for the bowel or bladder to recover, and around 6,500 of the 21,000 yearly stoma surgeries are permanent. Adapting to life with a stoma can be very difficult, not only affecting someone physically, but also contributing to self esteem issues, meaning that many may avoid certain activities out of fear associated with their stoma. Massage is an example of one of these activities, but there is no reason why a stoma should come between someone and their relaxation time.
TYPES OF STOMA
There are 3 types of stoma:-
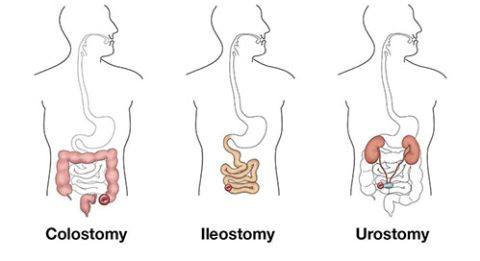
1)COLOSTOMY - approximately 65,000 out of 120,000 in UK
⦁ an opening in the large intestine, is created by bringing the healthy end of the colon through an incision in the abdominal wall
⦁ provides an alternative means for faeces to be excreted, either to allow the bowel to rest temporarily, or to act as a permanent artificial anus eg.in cases of ulcerative colitis or colorectal cancer
2)ILEOSTOMY - approximately 45,000 out of 120,000 in UK
⦁ opening of the small intestine, created by bringing the ileum to the surface of the skin, usually on the right side just above the groin
⦁ allows intestinal waste to be excreted before reaching the colon
3)UROSTOMY - approximately 10,000 out of 120,000 in UK
⦁ creates an opening to accommodate urinary diversion where drainage via the bladder and urethra is not possible, e.g. in cases of bladder cancer
BENEFITS OF MASSAGE FOR CLIENTS WITH A STOMA
Aside from all the usual benefits of massage that I talk about, there are some ways that massage can particularly benefit the person with a stoma.
⦁ helping to improve self esteem and body image
⦁ reducing the risk of adhesions after surgery - keeps the tissues moving so that they dont stick together
⦁ breaking down scar tissue in the later stage of the healing process
⦁ potentially can help to reduce the risk of post-surgical bowel blockages
⦁ assisting not only with passage of faeces, but also with wind, which can reduce pain
⦁ helps to maintain skin integrity
⦁ improving lymphatic circulation - oedema can be an issue in those with a stoma
LAYING FACE DOWN WITH A STOMA
Laying face down is probably the biggest obstacle that people feel stands in the way of getting a massage, but given that we, as therapists, adapt treatments and positioning for other reasons, eg. pregnancy or Down's syndrome, there is no reason why the same accommodation can't be given to a stoma. The body, and a stoma, can withstand pressure, but for clients who have recently acquired their stoma in particular, it can take some time to trust that this is the case.
There are various ways of adjusting positioning and each client will find what is comfortable for them:-
⦁ using the head cradle around the stoma, allowing the stoma bag to fall into the opening, so as not to prevent output, and pillows to support the other side of the body
⦁ use of a maternity pillow to lift the body around the stoma site
⦁ laying flat but the client places their hands under their hips to lift them up slightly
⦁ seated position
These measures can be more to offer emotional reassurance than anything else.
OTHER CONSIDERATIONS
⦁ while you don't have to tell the therapist that you have a stoma, they can give you a better treatment if they know. This is where seeing a therapist who has medical knowledge is recommended as they will understand the anatomy better and also the possible complications of having a stoma, and are not put off by 'medical imperfections'. Spa therapists whose focus is more beauty orientated would probably not be the best option.
⦁ feeling comfortable during a treatment is important so tell the therapist if something hurts, or doesn't feel right
For clients who have recently undergone surgery and are adjusting to life with a stoma, I would recommend taking a look at Mr Colitis Crohns. on social media, who has posted videos explaining the simple things that make life with a stoma a little easier. His insight into life with a stoma fills the gap from what you will be told by your medical team.
